Carpal tunnel syndrome often begins quietly. The earliest symptoms may seem minor — occasional numbness at night, brief tingling while driving, or a hand that feels like it “fell asleep.” Because these sensations are intermittent and painless at first, many people dismiss them.
Understanding the early signs of carpal tunnel syndrome allows for timely intervention, when symptoms are often reversible and permanent nerve damage can still be prevented.
1. What Is Carpal Tunnel Syndrome?
Carpal tunnel syndrome is a condition caused by compression of the median nerve as it passes through a narrow structure in the wrist called the carpal tunnel.
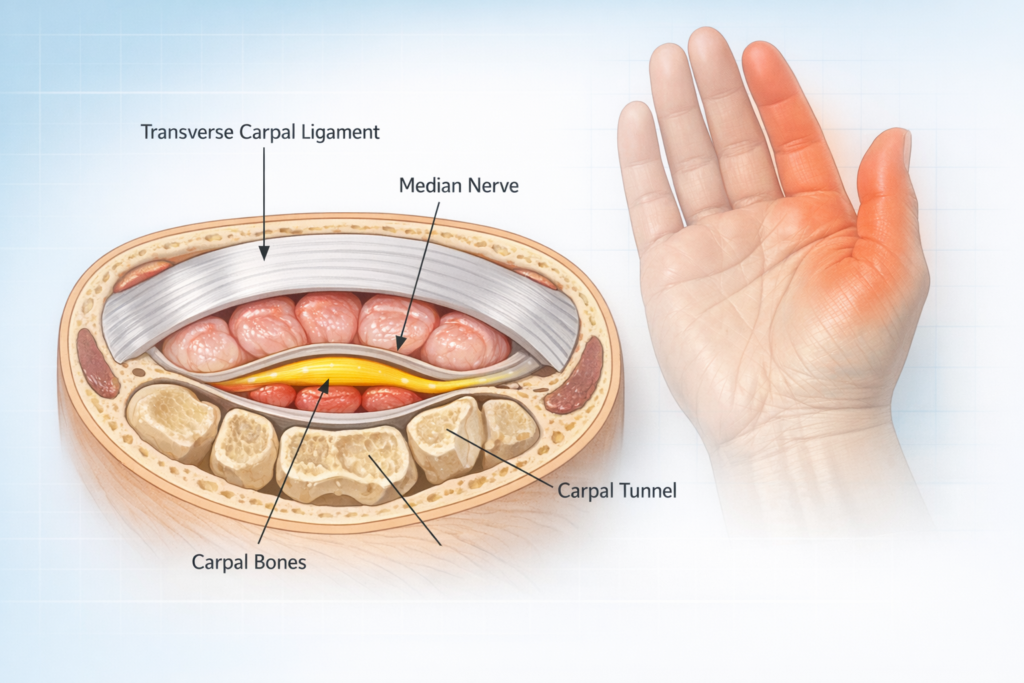
The carpal tunnel is a rigid, non-expandable passageway formed by:
- Carpal bones (floor and sides)
- Transverse carpal ligament (roof)
Inside this confined space run:
- The median nerve
- Nine flexor tendons
When pressure increases inside the tunnel, the median nerve becomes compressed. Because this nerve provides sensation to the thumb, index, middle, and part of the ring finger — and motor control to certain thumb muscles — symptoms follow a predictable pattern.
Why Symptoms Begin Subtly
Early compression primarily affects the nerve’s myelin sheath, the insulating layer responsible for fast signal conduction. At this stage:
- Signals become intermittently blocked
- Symptoms fluctuate
- Nerve fibers remain structurally intact
This is why early carpal tunnel can feel inconsistent rather than constant.
2. The Very First Early Signs of Carpal Tunnel
The earliest manifestations are usually sensory, intermittent, and often nocturnal.
Nighttime Numbness
One of the most common first symptoms is waking up with numbness in the hand.
Physiology:
- Wrist flexion during sleep increases tunnel pressure
- Venous congestion raises tissue swelling
- Median nerve conduction temporarily decreases
The result: numbness or tingling in the median nerve distribution.
Tingling in Thumb, Index, and Middle Fingers
The median nerve supplies sensation to:
- Thumb
- Index finger
- Middle finger
- Radial half of the ring finger
Tingling in this specific distribution is highly characteristic of carpal tunnel syndrome.
“Hand Falling Asleep”
Patients frequently describe:
- A “pins and needles” sensation
- A heavy or swollen feeling
- A need to shake the hand
This shaking temporarily improves blood flow and reduces mechanical compression, briefly restoring nerve conduction.
Temporary Relief After Shaking the Hand
The classic “flick sign” — shaking or flicking the wrist for relief — is strongly associated with early carpal tunnel.
Mechanism:
- Movement reduces intratunnel pressure
- Fluid redistributes
- Nerve signaling resumes
Intermittent Grip Weakness
Early motor involvement may manifest as:
- Dropping objects
- Difficulty opening jars
- Weak pinch strength
This reflects transient dysfunction of the thenar muscles, which are innervated by the median nerve.
Early Symptom Physiology Table
| Early Symptom | What’s Happening Inside the Nerve |
|---|---|
| Nighttime numbness | Temporary conduction block from increased tunnel pressure |
| Tingling fingers | Myelin irritation affecting sensory fibers |
| Hand “falling asleep” | Reduced nerve signaling due to compression |
| Relief with shaking | Pressure reduction restores conduction |
| Mild grip weakness | Early motor fiber dysfunction without axonal loss |
3. What Early Carpal Tunnel Feels Like (Real Sensory Description)
Patients often struggle to describe the sensation. Common descriptions include:
- “Pins and needles”
- Burning
- Electric shock–like sensation
- Crawling or buzzing feeling
- Tightness in fingers
Symptoms often worsen:
- At night
- While driving
- During prolonged typing
- When holding a phone
The discomfort is usually localized to the hand rather than the forearm or shoulder.
Addressing a Common Fear: “Could This Be ALS?”
It is common for individuals to worry about serious neurological diseases such as ALS.
Key distinctions:
Carpal tunnel syndrome:
- Causes sensory symptoms (numbness, tingling)
- Affects specific fingers
- Often worse at night
- Improves with shaking
ALS:
- Causes progressive motor weakness
- Does not cause sensory loss
- Involves multiple muscle groups
- Does not fluctuate
If numbness is present, ALS is highly unlikely. Sensory symptoms strongly favor peripheral nerve compression rather than motor neuron disease.
4. Why Symptoms Are Worse at Night
Nighttime worsening is one of the most important diagnostic clues.
Three mechanisms contribute:
1. Wrist Flexion During Sleep
Many people sleep with wrists bent. Flexion:
- Narrows the carpal tunnel
- Increases pressure on the median nerve
2. Fluid Redistribution
When lying flat:
- Interstitial fluid shifts toward extremities
- Tissue swelling increases inside the tunnel
3. Increased Tunnel Pressure
Studies show intratunnel pressure rises significantly during flexion and extension. The carpal tunnel cannot expand, so the nerve bears the pressure.
This explains why nighttime numbness is often the first sign of tunnel syndrome.
5. Early vs Advanced Carpal Tunnel Syndrome
Carpal tunnel progresses along a spectrum.
| Feature | Early Stage | Advanced Stage |
|---|---|---|
| Numbness | Intermittent | Constant |
| Pain | Mild or absent | Severe, persistent |
| Muscle weakness | Minimal | Significant |
| Muscle wasting | None | Thenar atrophy |
| Reversible? | Often yes | Sometimes permanent |
In early carpal tunnel, changes are primarily demyelinating. In advanced cases, axonal damage occurs, which may not fully recover even after treatment.
6. Risk Factors That Increase Your Chances
Certain risk factors increase the likelihood of developing carpal tunnel syndrome.
Modifiable
- Repetitive wrist motion
- Prolonged typing without ergonomic support
- Forceful gripping tasks
- Obesity
Non-Modifiable
- Pregnancy
- Diabetes
- Hypothyroidism
- Female sex
- Small wrist anatomy
Hormonal changes during pregnancy can increase fluid retention, temporarily narrowing the carpal tunnel.
7. Conditions Often Mistaken for Early Carpal Tunnel
Accurate differentiation is essential.
Arthritis
- Joint pain and stiffness
- Swelling localized to joints
- Does not follow median nerve distribution
Diabetic Neuropathy
- Symmetric numbness
- Affects both feet first
- Not confined to specific fingers
Cervical Radiculopathy
- Neck pain
- Radiation down arm
- Numbness follows dermatomal pattern
Cubital Tunnel Syndrome
- Affects ulnar nerve
- Numbness in ring and little finger
- Elbow-related compression
Distribution Comparison Table
| Condition | Thumb | Index | Middle | Ring | Little |
|---|---|---|---|---|---|
| Carpal tunnel | ✓ | ✓ | ✓ | Half | ✗ |
| Cubital tunnel | ✗ | ✗ | ✗ | Half | ✓ |
| Diabetic neuropathy | Diffuse | Diffuse | Diffuse | Diffuse | Diffuse |
| Cervical radiculopathy | Variable | Variable | Variable | Variable | Variable |
Correct anatomical distribution is a major diagnostic clue.
8. Can Early Carpal Tunnel Be Reversed?
In early carpal tunnel syndrome, nerve fibers are typically demyelinated but intact.
If compression is relieved:
- Myelin can regenerate
- Conduction velocity improves
- Symptoms resolve
Axonal damage, however, represents structural loss and may not fully recover.
Timeline of Recovery
- Mild cases: weeks to months
- After splinting or injection: days to weeks
- After surgery (if needed): months
Early intervention improves outcomes.
9. When to See a Doctor
Seek medical evaluation if:
- Symptoms last more than two weeks
- Nighttime numbness occurs daily
- You drop objects frequently
- Weakness progresses
- Thumb muscle appears smaller
Electrodiagnostic testing can confirm median nerve compression and assess severity.
10. Early Treatment Options
Early-stage treatment options are typically conservative.
Wrist Splints
Neutral-position splints worn at night:
- Prevent wrist flexion
- Reduce tunnel pressure
- Improve symptoms in many mild cases
Activity Modification
- Reduce repetitive strain
- Improve workstation ergonomics
- Avoid prolonged sustained wrist flexion
Ergonomic Adjustments
- Keyboard positioning
- Wrist support
- Break scheduling
Corticosteroid Injection
- Reduces inflammation
- Temporarily decreases pressure
- Effective in early inflammatory cases
Physical Therapy
- Nerve gliding exercises
- Postural correction
- Flexor tendon mobility work
Stage-based effectiveness is important: conservative treatment is most successful in early carpal tunnel syndrome.
11. Frequently Asked Questions
What were your first signs of carpal tunnel?
Most individuals report nighttime numbness, tingling in the thumb and first two fingers, and relief after shaking the hand. Symptoms are typically intermittent in early stages.
How do I test for carpal tunnel at home?
Simple maneuvers such as wrist flexion for 60 seconds (Phalen test) may reproduce symptoms. However, home testing is not diagnostic. A clinical exam and nerve conduction study provide confirmation.
Can carpal tunnel go away on its own?
Mild cases, especially those related to pregnancy or temporary overuse, may improve if pressure decreases. Persistent compression usually requires intervention.
Is numbness always serious?
Intermittent numbness is often reversible. Constant numbness or muscle weakness suggests more advanced nerve involvement and should be evaluated promptly.
Is pregnancy-related tunnel syndrome temporary?
Yes. Fluid retention during pregnancy can cause temporary compression. Symptoms often improve after delivery as swelling decreases.
How fast does it progress?
Progression varies. Some cases remain mild for years. Others worsen over months, especially if compression is continuous and untreated.
12. Key Takeaways
- Carpal tunnel syndrome begins subtly and often at night.
- Early symptoms include intermittent numbness and tingling in specific fingers.
- Nighttime worsening is due to wrist flexion and increased tunnel pressure.
- Sensory symptoms differentiate it from motor neuron diseases.
- Early stages are often reversible.
- Accurate differentiation from other nerve conditions is essential.
- Conservative measures are most effective when started early.
13. Medical Disclaimer
This article is for educational purposes only and does not constitute medical advice. If you are experiencing persistent numbness, weakness, or functional impairment, consult a qualified healthcare professional for individualized evaluation and management.